Getting a diagnosis
What the doctor may ask and why
If you see a doctor about the symptoms you have been having, they will ask you questions about:
- The symptoms you have e.g. cough, phlegm, breathlessness, number of infections and antibiotic courses.
- How long you have had these symptoms- sometimes people with bronchiectasis have symptoms for quite a while before a diagnosis.
- Any other medical problems you may have or medication you may take.
- Any family history of health problems.
- Your doctor will also need to ask you about smoking or contact with anything that can potentially affect people’s lungs. People with bronchiectasis have often never smoked, whereas some lung conditions are caused by smoking, so to make sure a correct diagnosis is made, it is important to ask.
- If a diagnosis of bronchiectasis is suspected, you will be referred to see a hospital doctor who specialises in this condition.
How you may feel
- Getting a diagnosis of bronchiectasis affects people differently and reactions can include disbelief, worry or even relief to have an explanation for your symptoms. Some people can feel frustrated if they have had symptoms for a long time.
- We interviewed patients to find out about their experiences of diagnosis and these are some of their thoughts:
“I was shocked but sort of glad in a way, because it explained why I hadn’t been well for so long” Tom, 33
“What first went through my mind…what caused it? Can it be cured? What does it mean for me?” Mike, 43
“Bronchiectasis… I just thought it was another word for ‘bronchitis’ really, I didn’t give it much more thought.” Paul, 75
“I often wonder “Did I have it when I was a child?” when I think back to different symptoms I had.” Shirley, 67
X rays and CT scans
- You are likely to have a chest X Ray performed first and then go on to have a CT scan of your lungs if bronchiectasis is suspected. This may be requested either by your GP, or when you attend your hospital clinic appointment.
- A chest X Ray may not necessarily show any changes in patients with bronchiectasis, and a CT scan is needed to confirm a diagnosis.
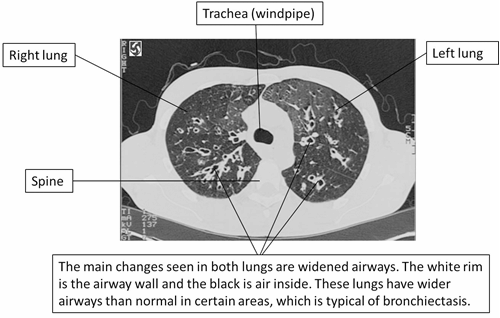
This is an image that you would get from having a CT scan of your lungs. These images are taken as ‘slices’ through the lungs and looked at as if looking up from your feet as you are lying down. Your doctor will be able to see any changes that are typically seen in bronchiectasis.
Breathing tests
Breathing tests
- These may also be called lung function tests, pulmonary function tests, or spirometry.
- Sometimes these can be done by your GP, but more often they are done at a hospital clinic by the lung function technician or lung physiologist or by the doctor.
- This test shows how well your lungs are functioning and can guide your treatment.
- Your results may be normal even if you do have bronchiectasis, or they may show some changes.
- You will probably repeat these tests each time you attend a clinic appointment so that your lung function and progress can be monitored.
Breathing tests are done using the machine pictured.

When you blow into the attached tube, the machine records how much air you can breath out in 1 second (FEV1 or Forced Expiratory Volume) and also when you breathe all the way out (FVC or Forced Vital Capacity). The machine produces a graph like the one below.
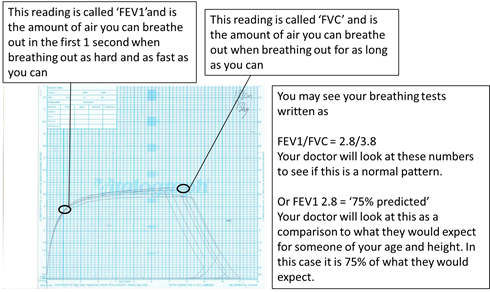
The results are then compared to what we would expect them to be for someone of your age and height. That way we can see if your lungs are working as well as they should be.
Sputum (phlegm) tests
- It is very important to be able to clear any phlegm from your chest, and also for samples to be regularly sent to the laboratory to be analysed.
- That way we can see which bugs may be present in the lungs, which can help to guide your treatment.
- You will be asked to give a phlegm sample in a sterile pot when you attend clinic.
- It is helpful if you can try to give a sample when you have an infection or flare up before you start a course of antibiotics to ensure you are on the correct treatment. You may start antibiotics before results are available, as these can take several days.
Blood tests
- When making a diagnosis of bronchiectasis, there are certain blood tests that need to be done. These are often done at your first hospital appointment, but may be done by your GP.
- After these initial blood tests, you will probably not need regular blood tests, just if there is a specific need. Some medications may require you have regular blood tests.
Your blood will be sent to:
Immunology
Checking your immune system and your body’s response to certain bacteria, vaccines and things you may be allergic to.
Haematology
Checking your blood cells.
Biochemistry
Checking your kidneys, liver and vitamin D levels.
Genetics
In certain situations more detailed genetic tests may be done.
More detailed tests
- Occasionally more detailed tests need to be done.
- This may include genetic tests or tests of how the cilia (tiny hairs within the lungs and airways) are working, depending on your age and family history, or special types of imaging, for example if you have been coughing blood (haemoptysis), or a camera test of the lungs called bronchoscopy. These are extra tests and are not done routinely. Your doctor will explain to you about these tests if you need to have them.
- The British Thoracic Society have guidelines for bronchiectasis that give details of what tests should be done and why. These guidelines are written for health care professionals rather than patients.
 Print
Print